Overview
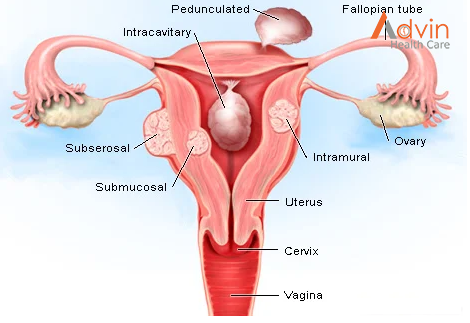
Vaginal hysterectomy is a surgical procedure to remove the uterus through the vagina.
During a vaginal hysterectomy, the surgeon detaches the uterus from the ovaries, fallopian tubes and upper vagina, as well as from the blood vessels and connective tissue that support it, before removing the uterus.
Vaginal hysterectomy involves a shorter time in the hospital, lower cost and faster recovery than an abdominal hysterectomy, which requires an incision in your lower abdomen. However, depending on the size and shape of your uterus or the reason for the surgery, vaginal hysterectomy might not be possible. Your doctor will talk to you about other surgical options, such as an abdominal hysterectomy.
Hysterectomy often includes removal of the cervix as well as the uterus. When the surgeon also removes one or both ovaries and fallopian tubes, it’s called a total hysterectomy with salpingo-oophorectomy. All of these organs are part of your reproductive system and are situated in your pelvis.
Types of hysterectomy
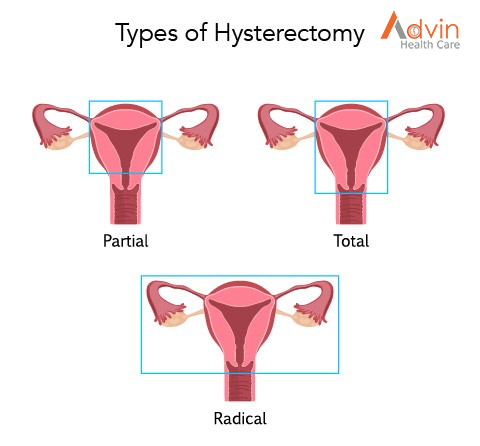
There are various types of hysterectomy. The type you have depends on why you need the operation and how much of your womb and surrounding reproductive system can safely be left in place
The main types of hysterectomy are:
total hysterectomy – the womb and cervix (neck of the womb) are removed; this is the most commonly performed operation
subtotal hysterectomy – the main body of the womb is removed, leaving the cervix in place.
total hysterectomy with bilateral salpingo-oophorectomy – the womb, cervix, fallopian tubes (salpingectomy) and ovaries (oophorectomy) are removed.
radical hysterectomy – the womb and surrounding tissues are removed, including the fallopian tubes, part of the vagina, ovaries, lymph glands and fatty tissue.
Why it’s done
Vaginal hysterectomy treats various gynaecological problems, including:
- Fibroids: Many hysterectomies are done to permanently treat these benign tumors in your uterus that can cause persistent bleeding, anemia, pelvic pain, pain during intercourse and bladder pressure. For large fibroids, you might need surgery that removes your uterus through an incision in your lower abdomen (abdominal hysterectomy).
- Endometriosis: This occurs when the tissue lining your uterus (endometrium) grows outside the uterus, involving the ovaries, fallopian tubes or other organs. Most women with endometriosis have a laparoscopic or robotic hysterectomy or abdominal hysterectomy, but sometimes a vaginal hysterectomy is possible.
- Adenomyosis: This occurs when the tissue that normally lines the uterus grows into the uterine wall. An enlarged uterus and painful, heavy periods result.
- Gynaecological cancer: If you have cancer of the uterus, cervix, endometrium or ovaries, or precancerous changes, your doctor might recommend a hysterectomy. Most often, treatment for ovarian cancer involves an abdominal hysterectomy, but sometimes vaginal hysterectomy is appropriate for women with cervical or endometrial cancer.
- Uterine prolapse: When pelvic supporting tissues and ligaments weaken or stretch out, the uterus can sag into the vagina, causing urine leakage, pelvic pressure or difficulty with bowel movements. Removing the uterus and repairing supportive tissues might relieve those symptoms.
- Abnormal uterine bleeding: When medication or a less invasive surgical procedure doesn’t control irregular, heavy or very long periods, hysterectomy may be needed.
- Chronic pelvic pain: If your pain is clearly caused by a uterine condition, hysterectomy might help, but only as a last resort. Chronic pelvic pain can have several causes, so an accurate diagnosis of the cause is critical before having a hysterectomy.
Laparoscopic or robotic hysterectomy
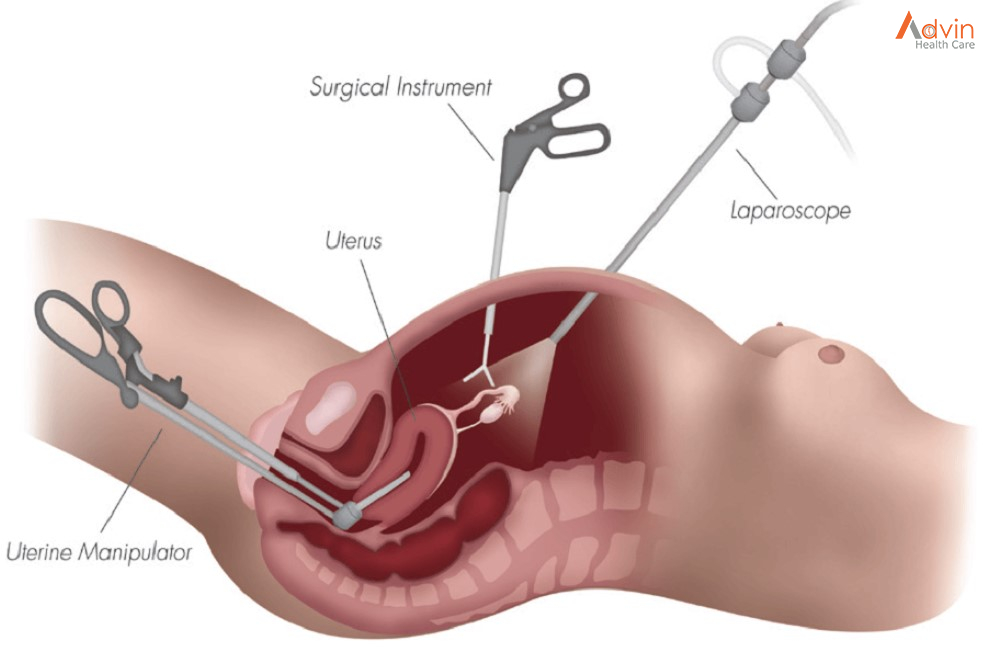
You might be a candidate for a laparoscopically assisted vaginal hysterectomy (LAVH) or robotic hysterectomy. Both procedures allow your surgeon to remove the uterus vaginally while being able to see your pelvic organs through a slender viewing instrument called a laparoscope.
Your surgeon performs most of the procedure through small abdominal incisions aided by long, thin surgical instruments inserted through the incisions. Your surgeon then removes the uterus through an incision made in your vagina.
Your surgeon might recommend LAVH or robotic hysterectomy if you have scar tissue on your pelvic organs from prior surgeries or from endometriosis.
Advantages of Vaginal hysterectomy Surgery
Minimally invasive laparoscopic hysterectomy produces excellent patient outcomes and offers many advantages over a traditional hysterectomy, including:
- Shorter hospital stays. In most cases, LH patients are discharged the same day or require an overnight stay, versus a three-to-four-day stay for traditional hysterectomy patients.
- Little to no blood loss as a result of smaller, shallower incisions.
- Lower risk of abdominal infection and other complications.
- Less pain. Patients generally can use a non-narcotic pain reliever if one is needed, as opposed to IV morphine or other prescription painkillers often given to patients who have a traditional hysterectomy.
- Faster recovery time. LH patients typically return to normal activities within one to two weeks, compared to four to six weeks for traditional hysterectomy.
- Minimal scarring. In many patients the scars become virtually unnoticeable.
Laparoscopic Vaginal Hysterectomy Products
- Laparoscopic Grasper
- Vessel Sealer Cutter
- Multifunction Trocar
- Laparoscope
- Monopolar scissor
- Veress Needle
- Uterine Manipulator
- Monopolar Electrodes
- Bissinger Bipolar Grasper
- Suction Irrigation Set
- Laparoscopy Trolley
- Endoscope Camera System
- Co2 Insufflator
- Electrosurgical Unit
- LED Light Source
- Video Recorder