Cataract Surgery
Cataract surgery is a procedure to remove the lens of your eye and, in most cases, replace it with an artificial lens. Normally, the lens of your eye is clear. A cataract causes the lens to become cloudy, which eventually affects your vision.
Cataract surgery is performed by an eye doctor (ophthalmologist) on an outpatient basis, which means you don’t have to stay in the hospital after the surgery. Cataract surgery is very common and is generally a safe procedure.
How long does cataract surgery take?
Cataract surgery takes 10 to 20 minutes to complete, depending on the severity of the condition. You should also plan to spend up to 30 minutes following the surgery to recover from the effects of the sedative.
Types of Cataract Surgery
There are two types of cataract surgery. Your doctor can explain the differences and help determine which is better for you:
- Phacoemulsification, or phaco. A small incision is made on the side of the cornea, the clear, dome-shaped surface that covers the front of the eye. Your doctor inserts a tiny probe into the eye. This device emits ultrasound waves that soften and break up the lens so that it can be removed by suction. Most cataract surgery today is done by phacoemulsification, also called “small incision cataract surgery.”
- Extracapsular surgery. Your doctor makes a longer incision on the side of the cornea and removes the cloudy core of the lens in one piece. The rest of the lens is removed by suction.
Prior to cataract surgery, antibiotic eye drops may be prescribed to prevent infection. Cataract surgery is most often done as an outpatient procedure with local anesthesia (a numbing gel is placed in the eye) and light intravenous sedation. You should not see instruments coming toward your eye and you should not feel pain in your eye during surgery. The incision made to remove the cataract is so small that it usually does not require stitches. Phacoemulsification (a type of ultrasound) is the most common method used to remove the cataract.
After the natural lens has been removed, it often is replaced by an artificial lens, called an intraocular lens (IOL). An IOL is a clear, plastic lens that requires no care and becomes a permanent part of your eye. Light is focused clearly by the IOL onto the retina, improving your vision. You will not feel or see the new lens.
Some people cannot have an IOL. They may have another eye disease or have problems during surgery. For these patients, a soft contact lens, or glasses that provide high magnification, may be suggested.
Surgical Options – Intraocular Lens
(IOL) Although all intraocular lenses are used to restore clarity of vision, there are many intraocular lens choices available to patients today.
- Standard lens implants are monofocal, meaning they are designed to correct the vision at one focal length. If a patient chooses to have IOLs implanted that correct for distance vision in both eyes, they will most likely need glasses to read. Some patients opt for an IOL that corrects their vision for distance in one eye and an IOL that corrects their vision for near in the other eye.
- Premium IOLs include the presbyopia-correcting IOLs and the toric IOLs. The decision to use these lenses must be made on an individual basis.
- Presbyopia-correcting intraocular lenses are designed to correct for distance and near vision. The intended goal of these lenses is to decrease the need for glasses.
- Toric intraocular lenses are used for those patients with astigmatism. Astigmatism refers to an irregularity in the curvature of the cornea. Toric IOLs are designed to correct distance vision and astigmatism.
Who needs cataract surgery?
You may need cataract surgery if cataracts are causing vision problems that interfere with your activities, like driving or reading.
Your provider also may need to remove a cataract to see the back of your eye and help manage other eye conditions, such as:
- Age-related changes in the retina (the tissue at the back of the eye).
- Diabetes-related retinopathy, an eye condition affecting people with diabetes.
What happens before cataract surgery?
Before cataract surgery, your ophthalmologist:
- Will measure your eye to find the correct focusing power for your IOL.
- Will ask about medications you take.
- May prescribe eyedrops to prevent infection and reduce eye swelling.
What happens during cataract surgery?
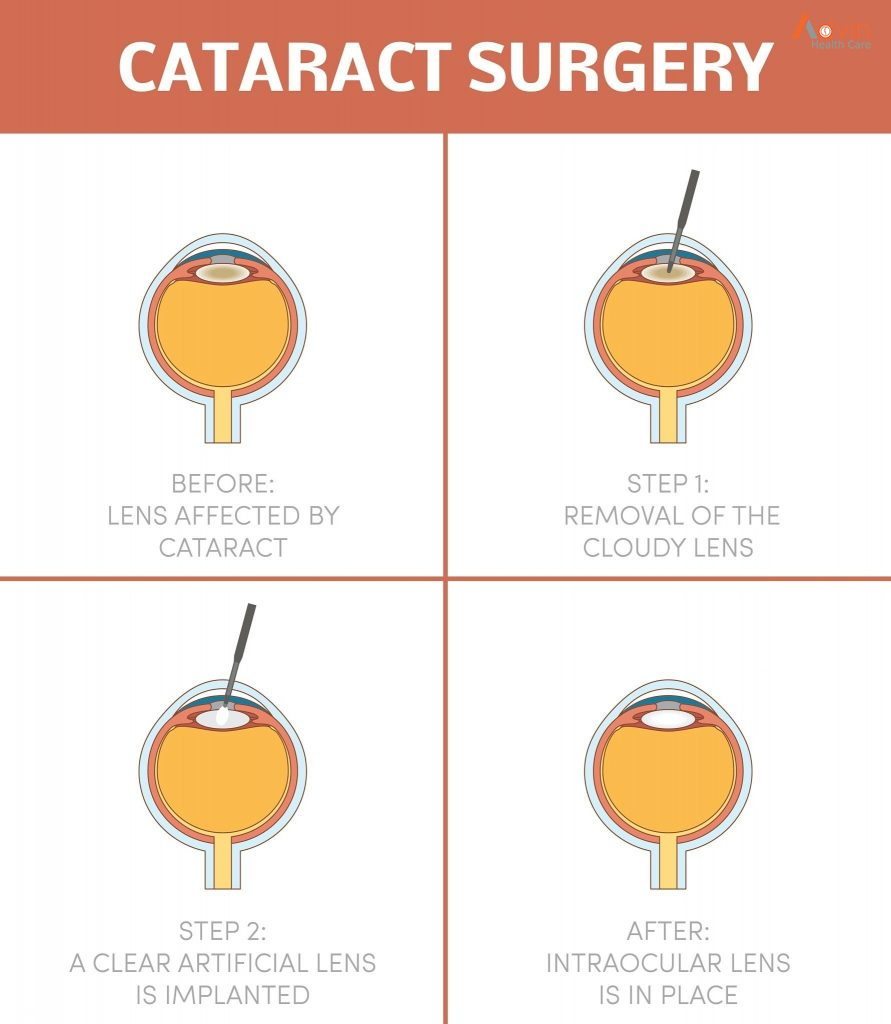
You may have to fast (not eat or drink) for a few hours before the surgery. Your provider may also ask you to stop taking certain medications for a few days.
Cataract surgery is an outpatient procedure, so you go home shortly after the surgery. You’ll need someone to come with you who can drive you home.
Here’s what to expect during the surgery:
- Numbing medication: Your provider numbs the eye with drops or an injection. You may also get medication to help you relax. You will be awake during the surgery and see light and movement. But you won’t see what the ophthalmologist is doing to your eye. The surgery won’t hurt.
- Cataract removal: Your provider uses a special microscope to see your eye. They create tiny incisions to reach the lens. Then they use ultrasound waves to break up the lens and remove it. Finally, they place the new lens.
- Recovery: You won’t need stitches. The tiny incisions close by themselves. Your provider will tape a shield (like an eye patch) over your eye to protect it.
What are the advantages of cataract surgery?
Cataract surgery is the only way to get rid of a cataract and sharpen your eyesight again. No other medicines or eyedrops are proven to improve cataracts.
Cataract surgery has a high success rate in improving people’s eyesight. Around 9 out of 10 people see better afterward.
After surgery, you can expect to:
- See things clearer.
- Have less glare when you look at bright lights.
- Tell the difference between colors.
ADVIN cataract instrument set
- Spatula Cum Y Rotator Double Ended
- Barraquer Wire Speculum Adult
- Barraquer Wire Speculum Child
- Barraquer Wire Speculum Infant
- IRIS Wire Retractor ST
- Caliper
- Capsule Polishing Curette
- Sinskey Hook
- Lens Loop Vectis
- IRIS Retractor Double Ended
- Smith Lens Expresser
- Hartman Mosquito Forceps
- Halstead Mosquito Forceps
- Botvin IRIS Forceps
- Corneal Forceps Toothed ST
- Limes Forceps Tooth
- Kelman McPherson IOL Forceps
- Tying Forceps ST
- Tying Forceps CVD
- Moorefield Conjunctival Forceps
- Fixation Forceps
- Superior Rectus Forceps
- Capsular Arruga Forceps
- Lens Holding Forceps
- Corneal Scissor CVD
- Westcott Tenotomy Scissor
- Vannes scissor Angled
- Castroviejo Needle Holder
- Cortex Cannula
- Simcoe Cannula
- BP Handle
- Sterilization Box with silicon Matt



