Introduction: Grasping Mechanism Defines Retrieval Efficiency
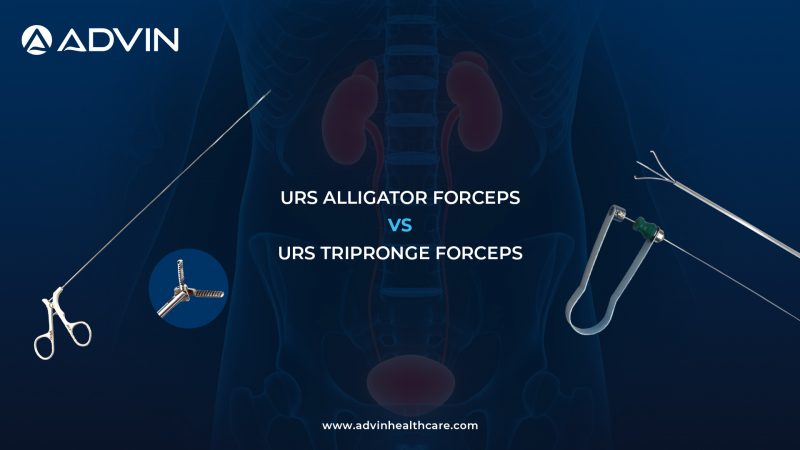
In endourology and endoscopic procedures, forceps are essential for grasping, holding, and retrieving foreign bodies or stones. The choice between Alligator Forceps and Triprong Forceps significantly affects grip strength, precision, and retrieval success.
While both instruments serve similar purposes, they differ in jaw design, holding mechanism, and clinical application.
Product Overview in Clinical Use
Alligator Forceps
Alligator Forceps are designed with long, narrow jaws that open vertically, similar to an alligator’s mouth.
Key characteristics:
- Serrated jaws
- Long, slim shaft
- Controlled opening mechanism
Clinical advantages:
- Strong and secure grip
- Precise handling in narrow spaces
- Suitable for linear or elongated objects
They are commonly used in foreign body retrieval and stone handling in confined areas.
Triprong Forceps
Triprong Forceps feature three-pronged jaws that open outward to grasp objects from multiple sides.
Key characteristics:
- Three flexible prongs
- Wide opening capability
- Multi-point contact
Clinical advantages:
- Better grip on irregular or round objects
- Increased surface contact
- Effective for loose or mobile stones
They are widely used in stone retrieval and grasping objects with uneven shapes.
Workflow-Based Usage: Firm Grip vs Multi-Point Capture
Both forceps are used for retrieval but differ in gripping style:
- Alligator Forceps → Linear, firm grip
- Triprong Forceps → Multi-directional grip
This impacts:
- Type of object handled
- Stability during extraction
- Ease of capture
Core Differences That Drive Clinical Choice
The key difference lies in jaw design and gripping mechanism:
- Alligator forceps offer precision and strong linear grip
- Triprong forceps provide multi-point grasping and better hold on irregular objects
Quick Comparison Overview
| Aspect | Alligator Forceps | Triprong Forceps |
|---|---|---|
| Jaw Design | Two serrated jaws | Three prongs |
| Grip Type | Linear grip | Multi-point grip |
| Precision | High | Moderate |
| Holding Strength | Strong | Moderate to strong |
| Object Type | Linear / firm objects | Round / irregular objects |
| Maneuverability | High in narrow spaces | Moderate |
| Clinical Use | Foreign body retrieval | Stone / fragment retrieval |
Clinical Preference & Real-World Application
Alligator Forceps are commonly used in:
- Foreign body removal
- Narrow anatomical pathways
- Situations requiring precise grip
Their design ensures secure and controlled handling.
Triprong Forceps are preferred in:
- Stone retrieval procedures
- Handling round or irregular objects
- Cases requiring multi-point grasp
Their structure ensures better capture and reduced slippage.
Practical Selection Guide
- Choose Alligator Forceps for precision and firm grip
- Choose Triprong Forceps for irregular objects and better capture
- Use alligator forceps in narrow spaces
- Use triprong forceps for stones and loose fragments
Conclusion: Precision vs Versatility in Gripping
Both instruments are essential in endoscopic retrieval:
- Alligator → Precise, strong, and controlled
- Triprong → Versatile, adaptive, and effective for irregular shapes
The ideal choice depends on:
- Type of object
- Anatomical location
- Required grip style
Why Advin Health Care is the Right Choice
Advin Health Care offers a complete range of retrieval forceps designed for precision and reliability.
- Alligator forceps provide strong grip and accurate handling
- Triprong forceps deliver versatile grasping and efficient retrieval
With Advin, healthcare providers benefit from:
- High-quality materials
- Durable construction
- Consistent clinical performance
Get Connected:
+91-70717 27261 | urology@advinhealthcare.com | www.advinhealthcare.com